Welcome to the Midwest Operating Engineers
Health Plan Marketplace
The goal of the Marketplace is to allow more choices to better meet our members’ health care needs while addressing rising health care costs for the Welfare Fund. The Marketplace enables you to choose an affordable plan that best meets your family’s needs which keeps more credits in your Credit Bank to extend your health plan coverage over time.
You can access the details of your health plan option by logging into your My150 account.
Open Enrollment occurs annually from mid- January through February. During this time, it’s important that you evaluate your projected work hours and your medical needs to ensure you are choosing a health plan option that best fits you and your family’s needs.
You are responsible for actively enrolling, through your My150 account, into a health plan option, either by selecting Start New Plan or Keep Current Plan, your newly validated dependents will be added to your coverage. If you do not actively select a health plan option and default, you will default into the same health plan option with the same dependents and no newly validated dependents will be added for coverage.
In January of each year, you will receive your open enrollment packet which will contain all the information that you will need in order to make an informed health care option decision. You can access the details of your health plan option by logging into your My150 account.
Under the MOE Health Plan Marketplace, after your first year of eligibility, you will have the opportunity to select from seven different health plan options. During Open Enrollment (mid-January through February), you can select a health plan option that best fits your family’s needs. This selected plan will be for coverage starting in the upcoming Plan Year (April 1 – March 31). Under the Marketplace, you also can choose your coverage tier; Member, Member + 1, Family.
Below is a chart of the health plan options, coverage tiers, and their associated monthly credit costs deductions. The monthly credit cost deductions are for the current 2023/2024 Plan Year and the 2024/2025 Plan Year. Monthly credit cost deductions are subject to change each Plan Year.
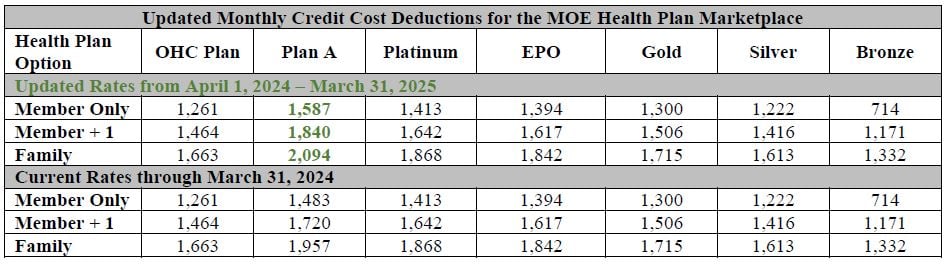
A credit is determined based on your Employer Contribution Rate less the Retiree Subsidy. The Retiree Subsidy is money that is used to supplement the Retiree Welfare Fund. The Retiree Subsidy for the 2023/2024 Plan Year is 17.3%. Therefore, a credit is determined as follows:
The chart below represents how the marketplace works after your first year of Eligibility.
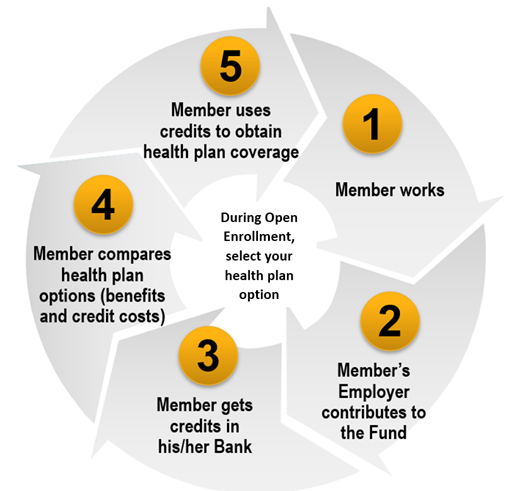
Under the MOE Health Plan Marketplace, there are a few ways to continue your eligibility under the Welfare Fund.
- Downgrades – You are allowed to downgrade once during each Plan Year for any reason. Plan Year for any reason. You may want to use this option if your work hours are slowing down, and you run the risk of depleting your Credit Bank. By choosing a downgrade, you are able to select a less costly health plan option. If you are a seasonal worker, you may want to select a downgrade so that you maintain your Welfare Fund coverage during the months that you are not working. By using this option, you are only allowed to change your health plan option to a lower costing health plan option; you are not allowed to change your coverage tier.
- Example 1: Suppose you are in Plan A, Family coverage tier. You would be allowed to choose from the remaining six options as all are less costly than Plan A.
- Example 2: Suppose you are in the Gold Plan, Member +1 coverage tier. You would be able to downgrade to either the OHC Plan, Silver, or Bronze Plan but remain in the Member +1 coverage tier.
Please note, if you transfer Plans, any amounts paid toward your deductibles or out-of-pocket maximums will be transferred to the new Plan.
- Self-Payments – You can make a one self-payment during each eligibility period. The self-payment will allow you to extend coverage for that one month that you are short credits. Example: Suppose you are in Plan A, Family coverage tier which has a monthly credit cost deduction of 1,957 credits. However, your current Credit Bank only has 1,200 credits. You could make a self-payment of $757.00 to remain covered under the Plan A, Family coverage tier for the one month.
- COBRA Coverage – If you decide to make the self-payment and are still not able to maintain coverage, you will be offered COBRA coverage. The Fund Office will send you a letter with all of the health plan options available to you and your eligible dependents. The member can select a lower costing health plan option/coverage tier; however, your dependents will have to pay for the same health plan option that they were previously covered under.
It is extremely important to maintain your eligibility under the MOE Health Plan Marketplace. If you lose your eligibility, you will need to re-establish your eligibility again by working the 300 hours in a consecutive 12-month period. Once you are eligible, you will be auto enrolled into the Bronze PPO plan. You will remain in that health plan option until the next Open Enrollment period. Also, depending on your age and when you are eligible to retire, this may affect whether you are eligible for the Retiree Welfare Plan (RWP) as you may jeopardize meeting the RWP service requirement for coverage. If you make the self-payment and/or select COBRA coverage, the months covered will be counted towards the RWP service requirements. If you have additional RWP eligibility questions, please call the Eligibility & Benefit Services Group at (708) 937-0327.
If you are considering retirement, it’s extremely important that you attend an open enrollment event prior to your selected retirement date.
This will be the last opportunity prior to retirement that you will be able to transfer credits from your Credit Bank to your Retiree Medical Savings Plan (RMSP) account. Recall your RMSP account can be used to pay for your Retiree Welfare Plan premium if you are eligible for the RWP. If you do not transfer enough credits during open enrollment, you will run out of your active credit bank until you transfer over to the RWP. When you become eligible for retiree coverage, you are no longer eligible for weekly disability, death benefits, or accidental dismemberment benefits (except Local 537; please call Fund Office for more information).
